Abstract
Purpose
To assess family satisfaction in the intensive care unit (ICU) and areas for improvement using quantitative and qualitative analyses.
Methods
Prospective cohort study performed in four (mixed surgical, neurological, and cardiological) intensive care units of a university hospital in Germany, using a translated and validated version of the Family Satisfaction in the ICU (FS-ICU) questionnaire, with questions answerable on a rating scale and three open-ended questions about strengths and weaknesses. Quantitative analysis was performed to identify items with low performance and high importance. For qualitative analysis, comments were coded and analyzed to identify important themes. Patient-related data were obtained from an electronic patient data management system.
Results
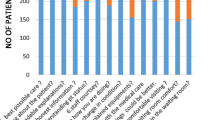
Participants were 215 family members visiting adult intensive care patients with length of stay over 48 h. Response rate was 28 %. Respondents were highly satisfied; summary scores were 78.3 ± 14.3 [mean ± standard deviation (SD)] on a scale of 0 (poor) to 100 (excellent). Regression analysis failed to identify association with patient- or family-related factors. The following themes for possible improvement emerged from both quantitative and qualitative analyses: patient agitation—consistency, clarity and completeness of information—emotional support—respect and compassion towards families. Families were also dissatisfied with the waiting room, ICU atmosphere, and amenities for visiting relatives.
Conclusions
Families report high satisfaction with intensive care. Nevertheless, there is room for improvement, in particular regarding how ICU staff communicate with families and provide emotional support.

Similar content being viewed by others
References
Institute of Medicine (2001) Crossing the quality chasm: a new health system for the 21st century. National Academy Press, Washington, DC
Kentish-Barnes N, Lemiale V, Chaize M, Pochard F, Azoulay E (2009) Assessing burden in families of critical care patients. Crit Care Med 37:S448–S456
de Vos M, Graafmans W, Keesman E, Westert G, van der Voort PH (2007) Quality measurement at intensive care units: which indicators should we use? J Crit Care 22:267–274
Heyland DK, Tranmer JE (2001) Measuring family satisfaction with care in the intensive care unit: the development of a questionnaire and preliminary results. J Crit Care 16:142–149
Wall RJ, Engelberg RA, Downey L, Heyland DK, Curtis JR (2007) Refinement, scoring, and validation of the Family Satisfaction in the Intensive Care Unit (FS-ICU) survey. Crit Care Med 35:271–279
Hekkert KD, Cihangir S, Kleefstra SM, van den Berg B, Kool RB (2009) Patient satisfaction revisited: a multilevel approach. Soc Sci Med 69:68–75
Stricker KH, Kimberger O, Schmidlin K, Zwahlen M, Mohr U, Rothen HU (2009) Family satisfaction in the intensive care unit: what makes the difference? Intensive Care Med 35:2051–2059
Heyland DK, Rocker GM, Dodek PM, Kutsogiannis DJ, Konopad E, Cook DJ, Peters S, Tranmer JE, O’Callaghan CJ (2002) Family satisfaction with care in the intensive care unit: results of a multiple center study. Crit Care Med 30:1413–1418
Dodek PM, Heyland DK, Rocker GM, Cook DJ (2004) Translating family satisfaction data into quality improvement. Crit Care Med 32:1922–1927
Henrich NJ, Dodek P, Heyland D, Cook D, Rocker G, Kutsogiannis D, Dale C, Fowler R, Ayas N (2011) Qualitative analysis of an intensive care unit family satisfaction survey. Crit Care Med 39:1000–1005
Dodek PM, Wong H, Heyland DK, Cook DJ, Rocker GM, Kutsogiannis DJ, Dale C, Fowler R, Robinson S, Ayas NT (2012) The relationship between organizational culture and family satisfaction in critical care. Crit Care Med 40:1506–1512
Stricker KH, Niemann S, Bugnon S, Wurz J, Rohrer O, Rothen HU (2007) Family satisfaction in the intensive care unit: cross-cultural adaptation of a questionnaire. J Crit Care 22:204–211
Huang R (2011) RQDA: R-based qualitative data analysis. R package version 0.2-1. http://rqda.r-forge.r-project.org/
Pope C, Ziebland S, Mays N (2000) Qualitative research in health care. Analysing qualitative data. BMJ 320:114–116
Stricker KH, Kimberger O, Brunner L, Rothen HU (2011) Patient satisfaction with care in the intensive care unit: can we rely on proxies? Acta Anaesthesiol Scand 55:149–156
Osborn TR, Curtis JR, Nielsen EL, Back AL, Shannon SE, Engelberg RA (2012) Identifying elements of ICU care that families report as important but unsatisfactory: decision-making control and ICU atmosphere. Chest 142(5):1185–1192
Rodriguez RM, Navarrete E, Schwaber J, McKleroy W, Clouse A, Kerrigan SF, Fortman J (2008) A prospective study of primary surrogate decision makers’ knowledge of intensive care. Crit Care Med 36:1633–1636
Peigne V, Chaize M, Falissard B, Kentish-Barnes N, Rusinova K, Megarbane B, Bele N, Cariou A, Fieux F, Garrouste-Orgeas M, Georges H, Jourdain M, Kouatchet A, Lautrette A, Legriel S, Regnier B, Renault A, Thirion M, Timsit JF, Toledano D, Chevret S, Pochard F, Schlemmer B, Azoulay E (2011) Important questions asked by family members of intensive care unit patients. Crit Care Med 39:1365–1371
Azoulay E, Pochard F, Chevret S, Lemaire F, Mokhtari M, Le Gall JR, Dhainaut JF, Schlemmer B (2001) Meeting the needs of intensive care unit patient families: a multicenter study. Am J Respir Crit Care Med 163:135–139
Puntillo KA, McAdam JL (2006) Communication between physicians and nurses as a target for improving end-of-life care in the intensive care unit: challenges and opportunities for moving forward. Crit Care Med 34:S332–S340
Krimshtein NS, Luhrs CA, Puntillo KA, Cortez TB, Livote EE, Penrod JD, Nelson JE (2011) Training nurses for interdisciplinary communication with families in the intensive care unit: an intervention. J Palliat Med 14:1325–1332
Curtis JR, Ciechanowski PS, Downey L, Gold J, Nielsen EL, Shannon SE, Treece PD, Young JP, Engelberg RA (2012) Development and evaluation of an interprofessional communication intervention to improve family outcomes in the ICU. Contemp Clin Trials 33(6):1245–1254
de Miranda S, Pochard F, Chaize M, Megarbane B, Cuvelier A, Bele N, Gonzalez-Bermejo J, Aboab J, Lautrette A, Lemiale V, Roche N, Thirion M, Chevret S, Schlemmer B, Similowski T, Azoulay E (2011) Postintensive care unit psychological burden in patients with chronic obstructive pulmonary disease and informal caregivers: a multicenter study. Crit Care Med 39:112–118
Pochard F, Azoulay E, Chevret S, Lemaire F, Hubert P, Canoui P, Grassin M, Zittoun R, le Gall JR, Dhainaut JF, Schlemmer B (2001) Symptoms of anxiety and depression in family members of intensive care unit patients: ethical hypothesis regarding decision-making capacity. Crit Care Med 29:1893–1897
Pochard F, Darmon M, Fassier T, Bollaert PE, Cheval C, Coloigner M, Merouani A, Moulront S, Pigne E, Pingat J, Zahar JR, Schlemmer B, Azoulay E (2005) Symptoms of anxiety and depression in family members of intensive care unit patients before discharge or death. A prospective multicenter study. J Crit Care 20:90–96
McAdam JL, Dracup KA, White DB, Fontaine DK, Puntillo KA (2010) Symptom experiences of family members of intensive care unit patients at high risk for dying. Crit Care Med 38:1078–1085
Jones C, Skirrow P, Griffiths RD, Humphris G, Ingleby S, Eddleston J, Waldmann C, Gager M (2004) Post-traumatic stress disorder-related symptoms in relatives of patients following intensive care. Intensive Care Med 30:456–460
Kross EK, Engelberg RA, Gries CJ, Nielsen EL, Zatzick D, Curtis JR (2011) ICU care associated with symptoms of depression and posttraumatic stress disorder among family members of patients who die in the ICU. Chest 139:795–801
Truog RD, Campbell ML, Curtis JR, Haas CE, Luce JM, Rubenfeld GD, Rushton CH, Kaufman DC (2008) Recommendations for end-of-life care in the intensive care unit: a consensus statement by the American College [corrected] of Critical Care Medicine. Crit Care Med 36:953–963
Davidson JE, Powers K, Hedayat KM, Tieszen M, Kon AA, Shepard E, Spuhler V, Todres ID, Levy M, Barr J, Ghandi R, Hirsch G, Armstrong D (2007) Clinical practice guidelines for support of the family in the patient-centered intensive care unit: American College of Critical Care Medicine Task Force 2004–2005. Crit Care Med 35:605–622
Lautrette A, Darmon M, Megarbane B, Joly LM, Chevret S, Adrie C, Barnoud D, Bleichner G, Bruel C, Choukroun G, Curtis JR, Fieux F, Galliot R, Garrouste-Orgeas M, Georges H, Goldgran-Toledano D, Jourdain M, Loubert G, Reignier J, Saidi F, Souweine B, Vincent F, Barnes NK, Pochard F, Schlemmer B, Azoulay E (2007) A communication strategy and brochure for relatives of patients dying in the ICU. N Engl J Med 356:469–478
Shelton W, Moore CD, Socaris S, Gao J, Dowling J (2010) The effect of a family support intervention on family satisfaction, length-of-stay, and cost of care in the intensive care unit. Crit Care Med 38:1315–1320
Hunziker S, McHugh W, Sarnoff-Lee B, Cannistraro S, Ngo L, Marcantonio E, Howell MD (2012) Predictors and correlates of dissatisfaction with intensive care. Crit Care Med 40:1554–1561
Wall RJ, Curtis JR, Cooke CR, Engelberg RA (2007) Family satisfaction in the ICU: differences between families of survivors and nonsurvivors. Chest 132:1425–1433
Sprung CL, Carmel S, Sjokvist P, Baras M, Cohen SL, Maia P, Beishuizen A, Nalos D, Novak I, Svantesson M, Benbenishty J, Henderson B (2007) Attitudes of European physicians, nurses, patients, and families regarding end-of-life decisions: the ETHICATT study. Intensive Care Med 33:104–110
Salandin A, Arnold J, Kornadt O (2011) Noise in an intensive care unit. J Acoust Soc Am 130:3754–3760
Konkani A, Oakley B (2011) Noise in hospital intensive care units-a critical review of a critical topic. J Crit Care 27:522, e521–e529
Kryworuchko J, Heyland DK (2009) Using family satisfaction data to improve the processes of care in ICU. Intensive Care Med 35:2015–2017
Acknowledgments
The CSCC is supported by the Federal Ministry of Education and Research (BMBF), Germany, FKZ: 01EO1002.
Conflicts of interest
The authors declare no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Trial registration: ClinicalTrials.gov Identifier NCT01449734.
Daniel Schwarzkopf and Susanne Behrend contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Schwarzkopf, D., Behrend, S., Skupin, H. et al. Family satisfaction in the intensive care unit: a quantitative and qualitative analysis. Intensive Care Med 39, 1071–1079 (2013). https://doi.org/10.1007/s00134-013-2862-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-013-2862-7