Abstract
Summary
The aim of this study was to investigate the association of surgical delay and comorbidities with the risk of mortality after hip fracture surgeries. We found that CCI was the dominant factor in predicting both short- and long-term mortality, and its effect is vital in the prognostication of survivorship.
Introduction
Hip fracture is a growing concern and a delay in surgery is often associated with a poorer outcome. We hypothesized that a higher Charlson Comorbidity Index (CCI) portends greater risk of mortality than a delay in surgery. Our aim was to investigate the associations of surgical delay and CCI with risk of mortality and to determine the dominant predictor.
Methods
This retrospective study examines hip fracture data from a large tertiary hospital in Singapore over the period January 2013 through December 2015. Data collected included age, gender, CCI, delay of surgery, fracture patterns, and the American Society of Anaesthesiologist (ASA) score. Post-operative outcomes analyzed included mortality at inpatient, at 30 and 90 days, and at 2 years.
Results
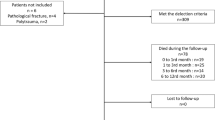
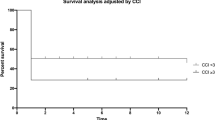
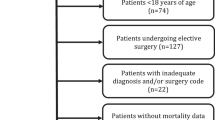
A total of 1004 patients with hip fractures were included in this study. Study mortality rates were 1.1% (n = 11) during in-hospital admission, 1.8% (n = 18) at 30 days, 2.7% (n = 27) at 90 days, and 13.3% (n = 129) at 2 years. Lost to follow-up rate at 2 years was 3.3%. We found that CCI was consistently the dominant factor in predicting both short- and long-term mortality. A CCI score of 5 was identified as the inflection point above which comorbidity at baseline presented a greater risk of mortality than a delay in surgery.
Conclusion
Our analysis showed that CCI is the dominant predictor of both short- and long-term mortality compared with delay in surgery. The effect of CCI is vital in the prognostication of mortality in patients surgically treated for hip fractures.


Similar content being viewed by others
References
Johnell O, Kanis JA (2006) An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int 17:1726–1733. https://doi.org/10.1007/s00198-006-0172-4
Johnell O (1997) The socioeconomic burden of fractures: today and in the 21st century. Am J Med 103:20S–25S discussion 25S-26S
Bentler SE, Liu L, Obrizan M, Cook EA, Wright KB, Geweke JF, Chrischilles EA, Pavlik CE, Wallace RB, Ohsfeldt RL, Jones MP, Rosenthal GE, Wolinsky FD (2009) The aftermath of hip fracture: discharge placement, functional status change, and mortality. Am J Epidemiol 170:1290–1299. https://doi.org/10.1093/aje/kwp266
Brauer CA, Coca-Perraillon M, Cutler DM, Rosen AB (2009) Incidence and mortality of hip fractures in the United States. JAMA 302:1573–1579. https://doi.org/10.1001/jama.2009.1462
Paksima N, Koval KJ, Aharanoff G et al (2008) Predictors of mortality after hip fracture: a 10-year prospective study. Bull NYU Hosp Jt Dis 66:111–117
Cooper C, Atkinson EJ, Jacobsen SJ, O’Fallon WM, Melton LJ III (1993) Population-based study of survival after osteoporotic fractures. Am J Epidemiol 137:1001–1005
Roche JJW, Wenn RT, Sahota O, Moran CG (2005) Effect of comorbidities and postoperative complications on mortality after hip fracture in elderly people: prospective observational cohort study. BMJ 331:1374. https://doi.org/10.1136/bmj.38643.663843.55
Doruk H, Mas MR, Yildiz C et al (2004) The effect of the timing of hip fracture surgery on the activity of daily living and mortality in elderly. Arch Gerontol Geriatr 39:179–185. https://doi.org/10.1016/j.archger.2004.03.004
Bottle A, Aylin P (2006) Mortality associated with delay in operation after hip fracture: observational study. BMJ 332:947–951. https://doi.org/10.1136/bmj.38790.468519.55
Al-Ani AN, Samuelsson B, Tidermark J et al (2008) Early operation on patients with a hip fracture improved the ability to return to independent living. A prospective study of 850 patients. J Bone Joint Surg Am 90:1436–1442. https://doi.org/10.2106/JBJS.G.00890
Grimes JP, Gregory PM, Noveck H, Butler MS, Carson JL (2002) The effects of time-to-surgery on mortality and morbidity in patients following hip fracture. Am J Med 112:702–709
Majumdar SR, Beaupre LA, Johnston DWC, Dick DA, Cinats JG, Jiang HX (2006) Lack of association between mortality and timing of surgical fixation in elderly patients with hip fracture: results of a retrospective population-based cohort study. Med Care 44:552–559. https://doi.org/10.1097/01.mlr.0000215812.13720.2e
Dailiana Z, Papakostidou I, Varitimidis S et al (2013) Surgical treatment of hip fractures: factors influencing mortality. Hippokratia 17:252–257
Bass E, French DD, Bradham DD, Rubenstein LZ (2007) Risk-adjusted mortality rates of elderly veterans with hip fractures. Ann Epidemiol 17:514–519. https://doi.org/10.1016/j.annepidem.2006.12.004
Kirkland LL, Kashiwagi DT, Burton MC, Cha S, Varkey P (2011) The Charlson Comorbidity Index score as a predictor of 30-day mortality after hip fracture surgery. Am J Med Qual 26:461–467. https://doi.org/10.1177/1062860611402188
de Souza RC, Pinheiro RS, Coeli CM, de Camargo KR (2008) The Charlson comorbidity index (CCI) for adjustment of hip fracture mortality in the elderly: analysis of the importance of recording secondary diagnoses. Cad Saude Publica 24:315–322
Neuhaus V, King J, Hageman MG, Ring DC (2013) Charlson comorbidity indices and in-hospital deaths in patients with hip fractures. Clin Orthop 471:1712–1719. https://doi.org/10.1007/s11999-012-2705-9
Lakomkin N, Kothari P, Dodd AC, VanHouten JP, Yarlagadda M, Collinge CA, Obremskey WT, Sethi MK (2017) Higher Charlson Comorbidity Index scores are associated with increased hospital length of stay after lower extremity orthopaedic trauma. J Orthop Trauma 31:21–26. https://doi.org/10.1097/BOT.0000000000000701
Lau TW, Fang C, Leung F (2016) Assessment of postoperative short-term and long-term mortality risk in Chinese geriatric patients for hip fracture using the Charlson comorbidity score. Hong Kong Med J Xianggang Yi Xue Za Zhi 22:16–22. https://doi.org/10.12809/hkmj154451
Bohl DD, Shen MR, Hannon CP, Fillingham YA, Darrith B, Della Valle CJ (2017) Serum albumin predicts survival and postoperative course following surgery for geriatric hip fracture. J Bone Joint Surg Am 99:2110–2118. https://doi.org/10.2106/JBJS.16.01620
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619
Charlson M, Szatrowski TP, Peterson J, Gold J (1994) Validation of a combined comorbidity index. J Clin Epidemiol 47:1245–1251
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Charlson ME, Sax FL, MacKenzie CR et al (1987) Morbidity during hospitalization: can we predict it? J Chronic Dis 40:705–712
Folbert EC, Hegeman JH, Vermeer M, Regtuijt EM, van der Velde D, ten Duis HJ, Slaets JP (2017) Improved 1-year mortality in elderly patients with a hip fracture following integrated orthogeriatric treatment. Osteoporos Int 28:269–277. https://doi.org/10.1007/s00198-016-3711-7
Lin JC-F, Liang W-M (2017) Mortality, readmission, and reoperation after hip fracture in nonagenarians. BMC Musculoskelet Disord 18. https://doi.org/10.1186/s12891-017-1493-5
Moja L, Piatti A, Pecoraro V et al (2012) Timing matters in hip fracture surgery: patients operated within 48 hours have better outcomes. A meta-analysis and meta-regression of over 190,000 patients. PLOS ONE 7:e46175. https://doi.org/10.1371/journal.pone.0046175
Uzoigwe CE, Burnand HGF, Cheesman CL, Aghedo DO, Faizi M, Middleton RG (2013) Early and ultra-early surgery in hip fracture patients improves survival. Injury 44:726–729. https://doi.org/10.1016/j.injury.2012.08.025
Orosz GM, Magaziner J, Hannan EL, Morrison RS, Koval K, Gilbert M, McLaughlin M, Halm EA, Wang JJ, Litke A, Silberzweig SB, Siu AL (2004) Association of timing of surgery for hip fracture and patient outcomes. JAMA 291:1738–1743. https://doi.org/10.1001/jama.291.14.1738
Moran CG, Wenn RT, Sikand M, Taylor AM (2005) Early mortality after hip fracture: is delay before surgery important? J Bone Joint Surg Am 87:483–489. https://doi.org/10.2106/JBJS.D.01796
Elkbuli A, Eily A, Polcz V, Boneva D, Spano II PJ, McKenney M, Hai S (2018) Isolated hip fracture in the elderly and time to surgery: is there an outcome difference? Trauma Surg Acute Care Open 3:e000212. https://doi.org/10.1136/tsaco-2018-000212
Pincus D, Ravi B, Wasserstein D, Huang A, Paterson JM, Nathens AB, Kreder HJ, Jenkinson RJ, Wodchis WP (2017) Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA 318:1994–2003. https://doi.org/10.1001/jama.2017.17606
Öztürk B, Johnsen SP, Röck ND, Pedersen L, Pedersen AB (2019) Impact of comorbidity on the association between surgery delay and mortality in hip fracture patients: a Danish nationwide cohort study. Injury 50:424–431. https://doi.org/10.1016/j.injury.2018.12.032
Klestil T, Röder C, Stotter C, Winkler B, Nehrer S, Lutz M, Klerings I, Wagner G, Gartlehner G, Nussbaumer-Streit B (2018) Impact of timing of surgery in elderly hip fracture patients: a systematic review and meta-analysis. Sci Rep 8:13933. https://doi.org/10.1038/s41598-018-32098-7
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study (CRIB Ref: 2015/2134) was approved by the SingHealth Centralised Institutional Review Board, Singapore.
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cher, E.W.L., Allen, J.C., Howe, T.S. et al. Comorbidity as the dominant predictor of mortality after hip fracture surgeries. Osteoporos Int 30, 2477–2483 (2019). https://doi.org/10.1007/s00198-019-05139-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05139-8