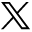Case presentation
A patient with a history of diverticulitis and cholelithiasis presented to hospital with approximately 24 hours of progressively worsening left-sided abdominal pain and intermittent obstipation. Physical examination revealed an afebrile, hemodynamically normal, well-appearing woman with mild left lower quadrant tenderness. Laboratory studies demonstrated modest leukocytosis (white cell count 11.0×109/L). CT of the abdomen and pelvis with intravenous contrast demonstrated a large bowel obstruction secondary to a cholecystocolonic fistula (CCF) with a 4.5-centimeter stone impacted in the descending colon (figure 1).
Coronal slices of admission CT of the abdomen/pelvis with intravenous contrast: (A) pneumobilia with associated thickening and inflammation of hepatic flexure; (B) large gallstone impacted in descending colon.
The patient was admitted to the surgical service for attempted non-operative management with nasogastric decompression, bowel rest, and maintenance fluids. After 48 hours, the stone remained impacted in the sigmoid colon on serial plain films. Subsequent endoscopic removal and lithotripsy were attempted by the gastroenterology service, but unsuccessful due to the presence of a diverticular stricture.
What would you do?
Exam under anesthesia (EUA) with attempted stone retrieval
Laparoscopic-assisted colotomy, stone removal and primary anastomosis
Sigmoid resection with primary anastomosis
Sigmoid resection and cholecystectomy
What we did and why
The patient was deemed to have failed non-operative management and the patient was brought to the operating room. We first attempted laparoscopic-assisted flexible sigmoidoscopy, where the primary surgeon manually attempted to milk the stone forward under visualization, with a second surgeon performing on table flexible sigmoidoscopy. Due to the large size of the stone, the stone could not be successfully dislodged, and thus the sigmoid was mobilized medially and brought up through a limited midline incision. A colotomy was made proximal to the point of impaction and a fully intact 4.5-centimeter gallstone removed (figure 2). The sigmoid stricture appeared benign and patent, and thus the sigmoid colon was left in situ. The colotomy was repaired transversely primarily in two layers with 3-0 Vicryl suture (inner running layer and an outer Lembert closure) and a subsequent leak test was negative. Severe right upper quadrant inflammation precluded safe cholecystectomy and fistula takedown. The patient was discharged home on postoperative day 4 after an uneventful recovery and seen follow-up at 1 month without any residual issues.
Intact, approximately 4.5-centimeter gallstone surgically extracted from sigmoid colon via proximal cololithotomy.
Discussion
CCF is a late complication of chronic cholelithiasis, affecting approximately 1 in every 1000 such cases.1 It most commonly affects women in the seventh to eighth decades of life, often with significant comorbid disease. Behind cholecystoduodenal fistula, CCF is the second most common presentation of cholecystoenteric fistula, representing anywhere from 8% to 26% of such cases. Symptoms are usually quite non-specific with approximately 25% of patients reporting chronic diarrhea. However, in the acute care setting, it represents approximately 4% of biliary ileus cases and less than 5% of all intestinal obstructions.2 3 Colon impaction, which most commonly occurs at the sigmoid colon, is additionally associated with gallstones greater than 2 cm in size and underlying colonic abnormality, usually diverticular disease.
Historically, CCF was commonly diagnosed intraoperatively at the time of planned cholecystectomy. CT of the abdomen/pelvis with intravenous contrast is now considered the gold-standard diagnostic study. However, the classic triad of pneumobilia, bowel dilation, and an ectopic gallstone is observed in less than half of all cases, thus highlighting the ongoing need for appropriate clinical suspicion.2
Surgical repair is typically recommended for CCF, but there is no formalized consensus on management. Although attempts at non-operative management may be reasonable in select patients, approximately 74% will require surgical intervention.4 Case reports of attempted colonoscopic extractions have been described in clinically stable patients, although few are ultimately successful.2 4–6
Overall survival is 87%, but decreases substantially to 54% in the 21% of patients who present with obvious bowel ischemia or perforation.4 7 Of this subset who require emergent surgical intervention, the majority are managed with a colectomy and diverting stoma creation. In clinically stable patients who can be managed less urgently, conflicting data exist regarding the morbidity and mortality of enterolithotomy alone versus enterolithotomy plus cholecystectomy with fistula takedown.8 9 Any presence of bowel compromise warrants segmental resection with either primary anastomosis or diversion. Although some patients are brought back for a two-stage operation, it has been shown that leaving the gallbladder and fistula in situ is a safe and feasible option. If a patient’s comorbidities and physiology permit and there is not prohibitive cholecystocolonic inflammation present intraoperatively, we will consider a one-stage operation. Otherwise, we most commonly leave the CCF intact in the presence of significant inflammation, bowel ischemia or perforation as well as in frail or unstable patients. If we consider a two-stage operation in a surgically fit patient, the preference is to wait a minimum of 8–12 weeks to address the CCF itself to allow for some inflammatory resolution. Ultimately, both surgical and non-surgical care is likely best tailored to a patient’s physiology and comorbid disease as well as the surgeon’s preference and skill set.
Ethics statements
Patient consent for publication
Ethics approval
This case report was reviewed by our institution’s Ethics and Institutional Board and determined exempt from review given the anonymized nature of the case report.
Footnotes
Contributors AWK—data collection, literature review and article writing. RW—literature review and article revision. LT—literature review and article revision. LMK—critical revisions of the article and project supervision.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests None declared.
Provenance and peer review Commissioned; internally peer reviewed.
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.