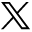Case presentation
A patient in their 60s with obesity (body mass index 49.3) presented with abdominal pain after a screening colonoscopy. At the outside hospital, a barium enema was performed which demonstrated extravasation of barium into the peritoneum. Figure 1A demonstrates the patient’s scout film from their CT abdomen/pelvis (CTAP) scan after barium enema. They were transferred to our quaternary referral center for emergent evaluation, and on arrival, they were afebrile and tachycardic. Abdominal examination demonstrated lower abdominal peritonitis and prominent ventral hernia with overlying skin changes. (figure 2A)
(A) Patient’s scout CT film on presentation to emergency department and (B) 1 month after initial operation.
Intraoperative photos including (A) external abdomen prior to exploratory laparotomy and (B) adherent serosal silver-white barium deposits present upon entry into the abdomen.
Immediately postcolonoscopy, what imaging study would you order for this patient?
CTAP with intravenous contrast
CTAP with oral contrast
CTAP with water-soluble contrast enema
CTAP with barium contrast enema
No imaging study needed, proceed for operative intervention.
What we did and why
We elected to promptly take the patient to the operating room for exploratory laparotomy given their examination, tachycardia, findings of barium throughout the peritoneum on preoperative imaging, and concern for ventral hernia strangulation with overlying skin changes and limited ability to evaluate bowel on preoperative CT related to the barium artifact. Prior to proceeding to the operating room, they were aggressively fluid resuscitated and given broad-spectrum antibiotics. Intraoperatively, findings included feculent peritonitis, colonic perforation with near-total coverage of intra-abdominal contents with barium contrast, necrotic and barium-coated omentum within the hernia sac, necrotic hernia skin, and ischemic small bowel within the hernia sac. Figure 2B demonstrates barium deposits present throughout the patient’s intestinal serosal surface.
Intraoperatively, their peritoneum was irrigated copiously with normal saline attempting to obtain source control. Barium deposits were meticulously removed both manually and using irrigation, taking great care to prevent mechanical trauma to the bowel serosa. It was noted that they had perforated at the site of a prior ileocolic anastomosis, although the patient had reported no prior abdominal operations on presentation. Therefore, a partial colectomy was performed, and they were left in discontinuity. The patient was hypotensive throughout most of the operation due to secondary effect of barium peritonitis and was resuscitated appropriately. After about 90 minutes of both irrigation and manual barium removal, due to the patient’s hemodynamics and the presence of dusky-appearing bowel versus reactive chemical irritation, the decision was made to place a temporary abdominal closure and return for a second look on postoperative day 2. At their operative takeback, they continued to have a large degree of barium peritonitis. The bowel was thoroughly inspected and additional necrotic bowel was resected leaving the patient with 180 cm of viable bowel. An ileocolic anastomosis and primary closure of the ventral hernia was performed. They tolerated the operation well and returned to the intensive care unit intubated. Postoperatively, the patient’s barium peritonitis resulted in prolonged ileus, requiring initiation of total parenteral nutrition and awaiting return of bowel function and eventual gastrostomy tube placement. They were subsequently discharged from the hospital almost 6 weeks from their index operation with barium still visible on CT imaging scount film (figure 1B).
This case demonstrates two major clinical challenges. The first challenge is selecting contrast to evaluate possible gastrointestinal abnormality. Benefits and drawbacks to both water-soluble contrast and barium are outlined in table 1. Although our center was not involved in the initial decision making, an evaluation for perforation demands a stepwise approach using water-soluble contrast or no enteral contrast. A CT scan with no contrast or intravenous contrast only would likely have sufficed in diagnosing perforation due to presence of pneumoperitoneum and/or free fluid.1 If no perforation is identified with water-soluble contrast, but clinical suspicion remains high, then barium (or water-soluble and barium mixture) may be used to rule out more subtle perforations, depending on the clinical scenario.
Benefits and drawbacks of using barium and water-soluble contrast
An additional challenge in this case rests in how to surgically decontaminate the peritoneal cavity. The current limited literature demonstrates that early laparotomy and washout/removal of barium from the peritoneum is beneficial as it can cause chemical peritonitis that can lead to fluid sequestration and hypovolemia.2 3 The optimal management strategy for removal of barium is unclear. Irrigation with normal saline is of some benefit, but due to barium’s adherent and accumulative nature, it is unlikely to be successful. Direct peritoneal lavage as part of temporary abdominal closure has not yet been described in the literature for barium peritonitis but could be considered and may have benefit.4 5 Furthermore, mechanical debridement risks injuring the serosal layer of the bowel and causing chemical irritation that can function similarly to leaving barium on the bowel. Long-term concerns include formation of adhesions due to barium residue on the intestinal serosa leading to recurrent bowel obstructions. Some authors advocate for omentectomy if necessary due to barium saturation to reduce risk of adhesions. The Closed Or Open after Laparotomy Trial seeks to clarify indications for a staged second-look surgery in the case of severe intra-abdominal sepsis using a prospective, randomized study design.6 7
Ethics statements
Patient consent for publication
Ethics approval
This study involves human participants. This study was exempt from Institutional Board approval as it is a case report. Patient consent was obtained and uploaded. Participants gave informed consent to participate in the study before taking part.
Footnotes
X @@ariananaaseh, @@jzaraterod, @GraceMNiziolek, @LKrankerMD
Collaborators Not applicable.
Contributors AN, JGZ, MJM, GMN, THN, JPK, LMK all contributed substantially to the conception of the work, drafting the work, and revising it for important intellectual content, and final approval of the version to be published.
Funding AN was supported by the Washington University School of Medicine Surgical Oncology Basic Science and Translational Research Training Program grant T32CA009621, from the National Cancer Institute (NCI). This content is solely the responsibility of the authors and does not represent the official view of the NCI.
Competing interests None declared.
Provenance and peer review Not commissioned; internally peer reviewed.
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.