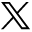Case presentation
An elderly patient in her 90s suffered an accidental fall at home 11 days prior to admission, resulting in hip pain and limited mobility of the right lower limb. She was able to walk with crutches before the incident. Her CT and X-ray (figure 1) demonstrated fracture of the superior/inferior pubis ramus and right ilium. The fracture was classified as type IIIa based on Rommens et al’s research.1 Blood gas analysis indicated low levels of Partial Pressure of Oxygen (PO2, 56.7 mm Hg) and Oxygen Saturation of blood (SaO2,90.9%; type 1 respiratory failure). Lumbar X-rays showed multiple old compression fractures of the thoracolumbar spine. Laboratory tests revealed hypokalemia (K+ of 3.37 mmol/L) and hypoproteinemia (Albumin, ALB of 31.4 g/L). In addition, the patient has a history of coronary heart disease, severe osteoporosis, and hypertension.
Preoperative (A) X-ray and (B, C) CT revealed a minimally displaced superior/inferior pubis ramus and right ilium (arrows).
What would you do?
Conservative treatment
Open reduction with internal fixation (ORIF)
Minimally invasive surgery manually
What we did and why?
To relieve her pain and immobilize the pelvis fracture, surgery was necessary. Considering the patient’s advanced age and comorbidities, the risks associated with ORIF are high. While minimally invasive surgery is a more suitable option, the risks of lumbar or general anesthesia is high. After careful discussion, we planned a robotic-assisted surgery under local anesthesia with percutaneous placement of osseous pathway screws, a technique that might reduce operation time.
The surgical procedure is shown in figure 2. The patient was placed supine, routinely sterilized, and taped. Local anesthesia was applied to the proximal part of the anterior superior iliac spine, followed by percutaneous placement of two 1.5 mm Kirschner wires for installation of the tracker. After three-dimensional (3D) CT scan, we planned the antegrade pubic screw and LC-II screw (a screw for the treatment of Young-Burgess LC type II pelvic fractures) using the Ti robot navigation system. The robot arm was then moved to the planned position, and the local anesthesia was applied and the guiding Kirschner wires for the screws were drilled into the bone. After confirmation of the position by X-ray, a 6.5×100 mm antegrade pubic screw and a 6.5×120 mm LC-II screw were inserted. A final 3D CT scan confirmed that the fracture alignment and the screw position were satisfactory. The wound was subsequently irrigated and sutured layer by layer.
Surgical procedure. (A) Procedure 1: tracker placement at the anterior superior iliac spine (arrow). (B) Procedure 2: intraoperative CT and three-dimensional plan of the iliac screw (left) and the superior pubic ramus screw (right). (C) Procedure 3: intraoperative confirmation of the screw after insertion.
Postoperative X-ray indicated that the screws were correctly positioned (figure 3). On the first day after surgery, the patient’s Visual Analog Scale(VAS) score decreased from 10 to 3. The patient was able to sit up at the bedside. On the third postoperative day, the patient was able to ambulate with crutches. The patient returned to preoperative level of activity at the 3-month postoperative follow-up (Majeed score 65, good).
Postoperative images showed that the screws are in the correct position. AP, anteroposterior.
Discussion
Patients with FFP endure a severe impact on their quality of life due to intense pain and loss of self-care capabilities.2 The goal of treating FFP is to achieve early fixation and functional exercise to restore independent daily activities.3 Notably, FFP typically arises from low-energy injuries. The fracture displacement is always limited as the ligaments around the pelvis in the elderly tend to be stronger than the bones, and the ligaments at the fracture site often remain intact after low-energy trauma. The treatment concept for FFP continues to evolve. Historically, FFP cases with minimal displacement were often managed conservatively, which requires prolonged bed rest, thus leading to respiratory, urinary, and other complications. After the introduction of the FFP classification system, Rommens et al1 recommended conservative treatment for type I/II fractures, while advising surgical intervention for type III/IV and type II fractures that fail conservative treatment.
Elderly pelvic fractures are common orthopedic injuries that can lead to significant morbidity and mortality. With increasing longevity, a growing geriatric population is vulnerable to lower-energy pelvic fractures.4 Most of the pelvic fractures among the geriatric population (age >60 years) are fragility fracture of the pelvis (FFPs). During the past decades, the incidence of FFP in older adults in the USA has increased by 24%, with a yearly increasing trend.5 Elderly FFP is characterized by high morbidity, mortality, and loss of independence.6
As anatomic reduction is no longer mandatory,3 7 some scholars think that the optimal strategy for treating FFP is minimally invasive surgery, which is also suggested by the AO group.8 9 Compared with conservative treatment, minimally invasive surgery, such as osseous fixation pathways, offers enhanced fracture stability, more favorable healing prospects, and improved functional recovery. Despite the advantages, accurate screw placement could be challenging, especially when dealing with displacement of FFP in the elderly, which can result in a narrowing of the bony channel. Even a 5 mm displacement in sacral fractures can reduce the S1 screw channel by 36%.10 Severe narrow bony channels, if left unaddressed, may lead to peripheral neurovascular injury as the screws penetrate the bone cortex, further complicating the procedure. Robotic assistance may enhance precision while allowing surgery under local anesthesia.
Numerous studies have compared the effects of surgical robots and manually placed screws for targeting pelvic fractures. A meta-analysis conducted by Al-Naseem et al11 indicated that the robot-assisted surgery exhibited advantages in terms of less operative duration, intraoperative bleeding, fluoroscopy exposure, and intraoperative drilling frequency when compared with conventional percutaneous sacroiliac screw fixation. Studies specifically involving robotic surgery for elderly patients with FFP remain limited. In this case, we performed percutaneous screw fixation under the guidance of Ti robot assistance and achieved favorable outcomes. The VAS score decreased from 10 to 3 after surgery. At the 3-month follow-up, the Majeed score reached 65, signifying a good outcome. The whole procedure holds many advantages. First, in comparison with non-operative treatment, the procedure allows for faster recovery and mobilization, thereby reducing the complications stemming from extended bed rest. Second, we only had to drill the guiding wire once under the navigation of the robot arm. The whole procedure lasts 60 minutes. In contrast to manual surgery, this method ensures accurate screw placement (thereby avoiding screw penetration), reduces surgical time, and minimizes radiation exposure. This was consistent with the result of Al-Naseem et al’s meta-analysis.11 Last, the surgery was conducted under local anesthesia, which mitigated the risk of complications associated with general anesthesia, such as postoperative confusion and hypoventilation. This approach expands the opportunity for more elderly patients with FFP with compromised systemic conditions to undergo surgical treatment.
To be noted, the process of acquiring the necessary skills becomes progressively challenging and time-consuming as surgeons have to master both anatomic knowledge and the basic principles of running the robotic system simultaneously. Furthermore, careful selection of indications is required as robots may not be currently suitable for all FFP cases, especially those involving complex and displaced pelvic fractures.
Conclusion
Using robotic assistance for minimally invasive treatment of pelvic fractures under local anesthesia provides a safe and effective option for selected patients. This is the first patient with FFP treated under local anesthesia. The robot system can aid in preoperative planning and intraoperative navigation, which sets the stage for local anesthesia. The procedure significantly improves accuracy and safety while reducing surgical duration.
Ethics statements
Patient consent for publication
Ethics approval
This study involves human participants and the case report was published with the consent of the patient. The participant gave informed consent to participate in the study before taking part.
Footnotes
Contributors YH L was the guarantor for this study. SoL conceptualized the case report and drafted the article. ShL performed the surgery, managed patient care, and contributed to data collection and article review. KX analyzed the data, conducted the literature review, and assisted with article writing and figure preparation. XW assisted in surgery, collected the data, and reviewed the article. YL provided supervision, assisted with data interpretation, and reviewed the article.
Funding This work was supported by grants from the scientific research fund of Aerospace Center Hospital (no: YN202303), Foundation of AMHT (2021YK17), Non-profit Central Research Institute Fund of Chinese Academy of Medical Sciences (2023-JKCS-26), Beijing Municipal Science and Technology Commission (no: Z221100007922003) and Beijing Natural Science Foundation (no: L222062).
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.